Silent Inflammation Is the Reason High Performers Break Without Warning
The labs came back normal. The patient is still declining. This is not a contradiction. It's a gap in what was measured.
This is the conversation I have most often with high-output professionals. Executives, surgeons, founders, athletes, parents who are running a business and a household at the same time. The labs say they are fine. Their body is telling them they are not. Both can be true at once when the markers being measured are not the markers that matter.
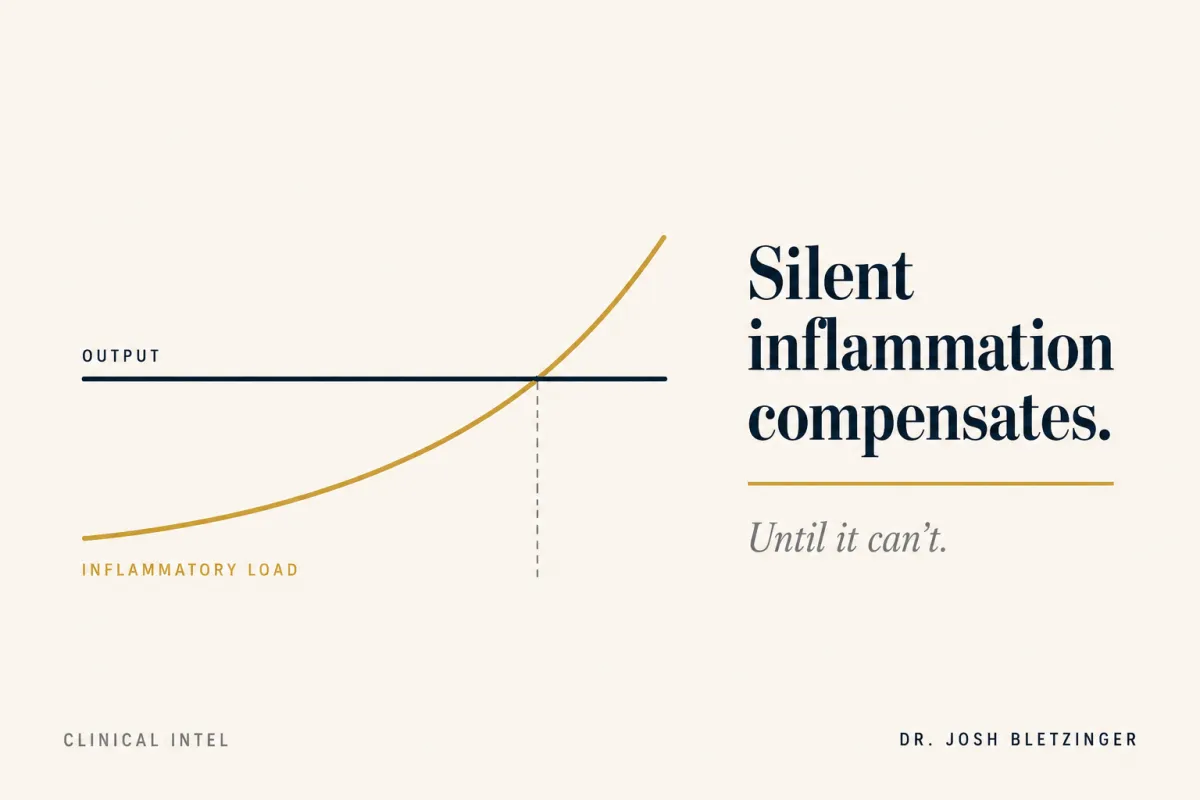
Silent inflammation is the most dangerous form of compensation. It performs normally until it doesn't.
The CRP Problem
Most standard panels include a single inflammation marker: C-reactive protein, measured at the standard sensitivity range. That assay was designed to flag acute inflammatory disease. Pneumonia. Rheumatoid flare. Active infection.
It was not designed to detect the chronic, low-grade systemic load that erodes performance in otherwise healthy adults. The threshold is too coarse. By the time a standard CRP reads high, the inflammatory load has been compounding for a long time. Often years.
Reading 'normal' on standard CRP does not mean inflammation is absent. It means it's below the threshold of a tool built to catch a different problem.
What hs-CRP Actually Tells You
High-sensitivity CRP is the same protein, measured with a more granular assay. It can resolve values that the standard test cannot.
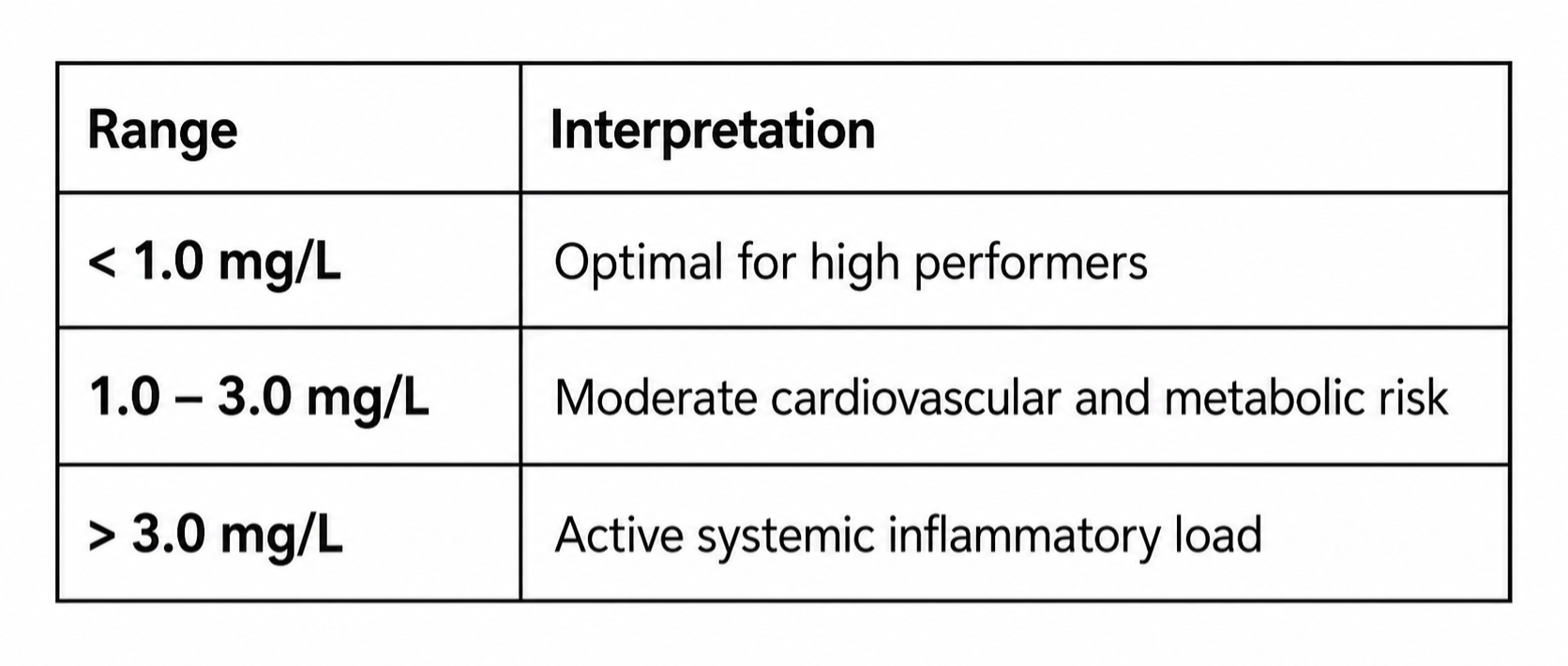
Clinically, the optimal range for a high performer sits at less than 1.0 mg/L. The 1.0 to 3.0 range is moderate cardiovascular and metabolic risk. Above 3.0 indicates active systemic inflammatory load, even when the patient is asymptomatic.
The literature on hs-CRP and long-term cardiovascular risk is decades deep. What gets less attention is the relationship between subclinical hs-CRP elevation and the slow erosion of cognitive sharpness, recovery capacity, and metabolic flexibility in people who still feel mostly fine.
The inflammation is not loud. It's compounding quietly.
The Four Drivers Hiding in Plain Sight
In high-output individuals, four upstream sources account for the majority of silent inflammatory load. None of them are flagged on a standard panel.
Sleep debt and IL-6 elevation. A single night of partial sleep restriction elevates IL-6 the following day. Chronic sleep debt sustains that elevation. The patient does not feel acutely inflamed. The signal is running underneath everything else.
Gut permeability and LPS translocation. When the intestinal barrier is compromised, lipopolysaccharide from gram-negative bacteria translocates into systemic circulation. The immune system mounts a low-grade chronic response. Standard panels do not measure intestinal permeability. The patient has no GI complaints. The load is real anyway.
Overreaching without recovery. Training load is not the problem. Training load that exceeds adaptive capacity is the problem. When output keeps exceeding recovery, the inflammatory cost of the work compounds. The performance does not visibly drop right away. The capacity to recover from the next stressor does.
Dietary inflammation without obvious symptoms. Food sensitivities, refined seed oil load, glycemic volatility, alcohol clearance burden. None of these require an obvious GI or skin reaction to be elevating systemic inflammatory tone. They quietly raise the floor.
These four drivers stack. They do not present as four separate problems. They present as one trajectory.
What Performance Masking Looks Like
The reason this is so dangerous in high performers is the very thing that makes them effective. They have above-average capacity to override symptoms with structure. They sleep less and still execute. They train hard and still show up. They produce.
Output is not the same as capacity.
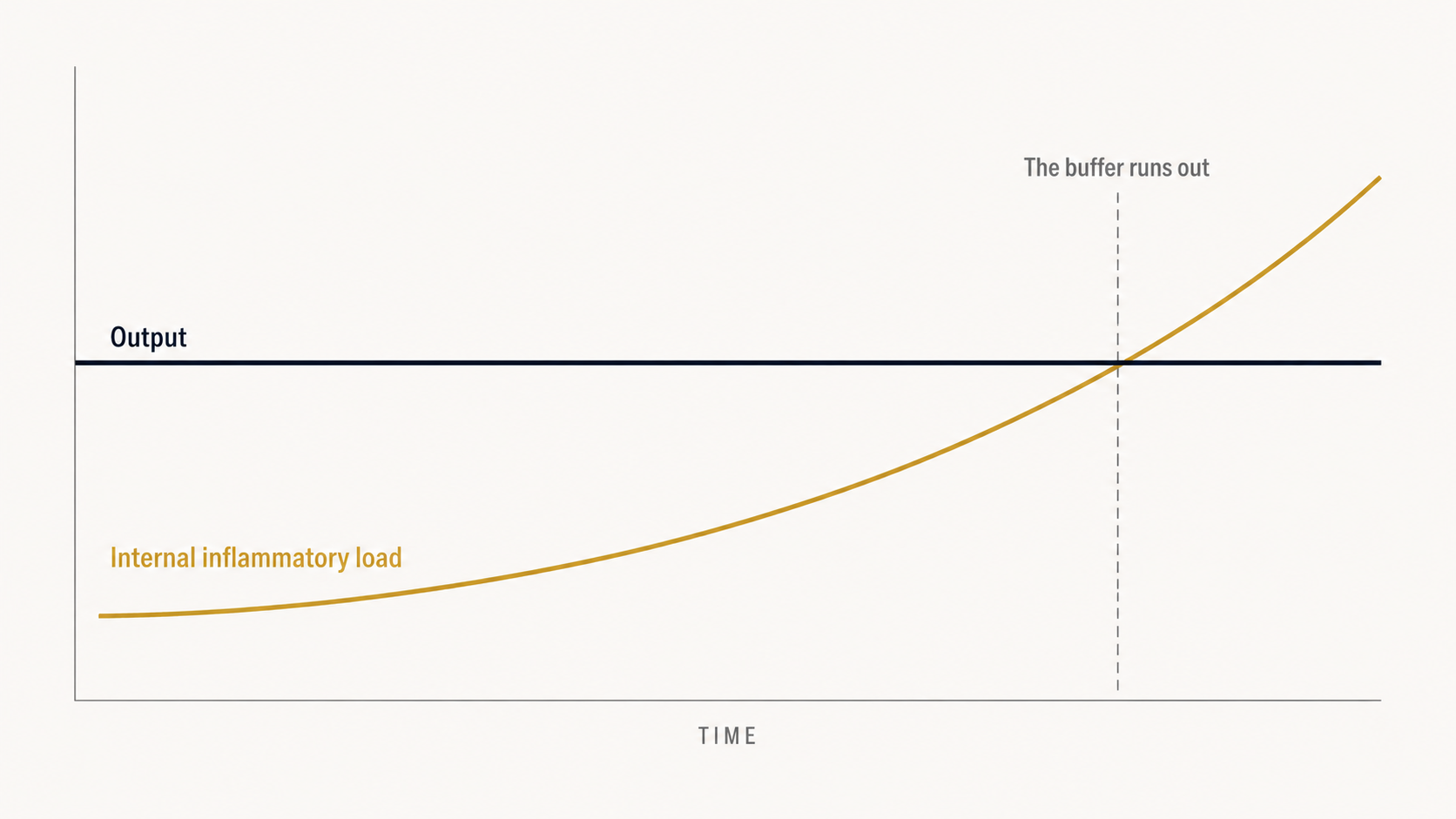
The output stays consistent. The internal load accumulates underneath it.
This is the compensation model. The body buffers, until the buffer is gone. The crash, the injury, the cardiac event, the sudden cognitive drop, the metabolic diagnosis that 'came out of nowhere,' all of these are the moment the buffer ran out. They were not sudden. They were the visible end of a long quiet process.
The Clinical Threshold and What to Add
If standard CRP is the only inflammation marker on your last panel, you do not have data on this question. You have the absence of acute disease, which is a different question entirely.
The minimum I want on a high performer is hs-CRP, ferritin, fasting insulin, HbA1c, and a homocysteine. From there, the panel expands based on the clinical picture: omega-3 index, GGT, oxidized LDL, intestinal permeability markers when indicated, and a deeper look at the HPA axis when the inflammatory pattern is downstream of allostatic load.
Retesting cadence matters. Inflammatory markers are not static. They are the running total of how the system is handling its current load. Trended over time, they are one of the most useful signals in functional medicine.
A More Complete Map
This is not about fear. It's about precision. A normal standard panel is not a clean bill of health. It is a small set of data points, interpreted against population averages, designed to flag overt disease.
If you're operating at the top of your field and feel like you are running at 80 percent of your own ceiling, the question is not whether something is wrong. The question is what your inflammatory load actually looks like at the resolution that matters.
That's what we measure. That's what we move.
Key Takeaways
A "normal" standard CRP does not rule out chronic inflammation. The standard assay was built to detect acute disease, not low-grade systemic load.
High-sensitivity CRP is the appropriate marker for high performers. Optimal is less than 1.0 mg/L.
Four upstream drivers account for most silent inflammatory load: sleep debt, gut permeability, training overreach, and dietary inflammation. None show up directly on a standard panel.
High performers mask inflammation through structure and output. The buffer holds until it doesn't. The 'sudden' event is rarely sudden.
The minimum panel for this question includes hs-CRP, ferritin, fasting insulin, HbA1c, and homocysteine. Trended over time, not measured once.
Next Steps
If you want a clinical map of your own inflammatory and metabolic load: the Performance Gap Diagnostic is the entry point. It pairs a structured symptom burden inventory with a functional blood chemistry panel, including the markers above. Performance Gap Diagnostic
If you want the broader framework first: the next live Performance Gap Live Training walks through the four systems and the compensation model in full.
The Performance Gap Live Training - May 30, 2026 - 10AM
References
Sleep debt and IL-6 elevation
Vgontzas AN, Zoumakis E, Bixler EO, et al. Adverse effects of modest sleep restriction on sleepiness, performance, and inflammatory cytokines. J Clin Endocrinol Metab. 2004;89(5):2119-2126. PMID: 15126529.
Irwin MR, Olmstead R, Carroll JE. Sleep disturbance, sleep duration, and inflammation: a systematic review and meta-analysis of cohort studies and experimental sleep deprivation. Biol Psychiatry. 2016;80(1):40-52. PMID: 26140821.
hs-CRP and cardiovascular / metabolic risk
Ridker PM. A test in context: high-sensitivity C-reactive protein. J Am Coll Cardiol. 2016;67(6):712-723. PMID: 26868696.
Pearson TA, Mensah GA, Alexander RW, et al. Markers of inflammation and cardiovascular disease: application to clinical and public health practice. AHA/CDC scientific statement. Circulation. 2003;107(3):499-511. PMID: 12551878.
Gut permeability and LPS translocation
Cani PD, Amar J, Iglesias MA, et al. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007;56(7):1761-1772. PMID: 17456850.
Camilleri M. Leaky gut: mechanisms, measurement and clinical implications in humans. Gut. 2019;68(8):1516-1526. PMID: 31076401.
Training overreach and inflammatory load
Smith LL. Cytokine hypothesis of overtraining: a physiological adaptation to excessive stress? Med Sci Sports Exerc. 2000;32(2):317-331. PMID: 10694113.
Meeusen R, Duclos M, Foster C, et al. Prevention, diagnosis, and treatment of the overtraining syndrome: joint consensus statement of the ECSS and ACSM. Med Sci Sports Exerc. 2013;45(1):186-205. PMID: 23247672.
Dietary inflammation
Shivappa N, Steck SE, Hurley TG, et al. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014;17(8):1689-1696. PMID: 23941862.
